Stolen Future: Part 1
What’s wrong with my brain?
About the series
Lonni Schicker, 64, was always the one to depend on, to get things done and to figure things out. She was the person who took care of others. At least until about five years ago, when Lonni's doctor told her that at age 59 she had mild cognitive impairment. The diagnosis placed her at higher risk of dementia. Lonni quit her job as a professor and moved into an apartment in Fenton with her son. Her problems have since gotten worse. Hoping to help others, Lonni is sharing her story about her frustrating search for a diagnosis and unique challenges when symptoms strike at a younger age.
Listen
Michele Munz reads the first story in her series about Lonni Schicker and her struggles with dementia. Lonnie is fighting to find out why her "brain doesn't work anymore."
She was the only patient in the small waiting room at Mercy Hospital. Calming scenes played on a small television screen — waterfalls, creeks flowing over rocks and leaves waving in sunlight.
Lonni Schicker, 63, took out a new journal and started writing in neat cursive: Seeing shadows. Paranoid. Lose balance. Can’t count change. Can’t remember email or text. Think Dan is tired of caring for me.
She’s about to see a neuropsychologist who is going to spend the next nearly four hours administering verbal and written tests for Dementia When problems with memory, language, thinking and judgment are greater than normal age-related changes. Problems aren't severe enough to significantly interfere with daily activities. A person with mild cognitive impairment is at increased risk of developing Alzheimer's or other dementia.dementia. She wants to make sure she tells him everything.
Lonni hopes that this time, she finally gets answers. She’s lost so much — her job as a college professor, her independence, her resilience.

While working as nurse and administrator, Lonni Schicker earned a bachelor's degree in 2000 and master's degree in health care management in 2004 from the University of St. Francis in Joliet. She is pictured here in the spring of 2011, earning her doctorate in education from Lindenwood University. She became a professor at Minnesota State University that fall. Photo courtesy of Lonni Schicker
Four years ago, at the age of 59, tests revealed Lonni had Mild cognitive impairment When problems with memory, language, thinking and judgment are greater than normal age-related changes. Problems aren't severe enough to significantly interfere with daily activities. A person with mild cognitive impairment is at increased risk of developing Alzheimer's or other dementia.mild cognitive impairment. Her neurologist wanted to monitor her.
Mild cognitive impairment is the gray area between normal functioning and dementia, which is the progressive decline in thinking skills great enough to hinder daily function.
With mild cognitive impairment, changes are serious enough to be noticed but don’t yet interfere with independence.
Mild impairment does not always lead to dementia. Sometimes, the condition gets better or stays the same. In other cases, it can be mistakenly diagnosed.
But about half the time, it can be the beginning of dementia. That means it will get worse, much worse.
Soon after her diagnosis, Lonni felt she could no longer handle the demands of being a professor. She worried about an uncertain future.

Lonni Schicker talks with her son, Dan Schicker, (left), and his friend Cameron Flood on Sunday Dec. 17, 2017, while she takes a break from cooking a big holiday meal for Dan and many of his friends. Christian Gooden / St. Louis Post-Dispatch
She abruptly retired and returned to her hometown to be near family. She moved into an apartment in Fenton with her son, Dan.
“If you're a patient, you just keep wondering, what the hell is wrong with me? You want it to have a name ... I want to know why my brain doesn't work anymore.”
Lonni’s symptoms have since gotten worse. With limited medical coverage, however, she has been left with more questions than answers.
Her Medicare coverage kicked in last spring, providing access to more consistent care. Her new neurologist ordered testing again, which brought her to the waiting room March 5.
Neuropsychologist John Wright opened the door. “Lonni?” he said, jokingly looking around. He tries to put patients at ease, especially ones like her, who take pride in their intellect. Because he’s about to challenge it.
Though Lonni was eager for answers, she was frustrated. She felt she was starting from scratch.
“It just makes me feel so stupid,” she said. “It makes me realize how far I’ve fallen.”
Lonni Schicker, a former professor, details her frustration at not being able to function like she used to. Her son, Dan, laments her having a condition that corrodes her most valued asset — her mind. (Cristina M. Fletes / St. Louis Post-Dispatch)
The path to a dementia diagnosis is often long and difficult, especially for those under the age of 65, when dementia is less common or in the early stages. Doctors and patients aren’t quick to consider the possibility.
With no simple diagnostic tool, figuring out the type of dementia can also be challenging. Alzheimer’s disease is the most common type — 60 percent to 75 percent of cases — but there’s also vascular dementia, frontotemporal and others. Sometimes, patients have a combination of types.
Symptoms may not neatly match a certain type, leaving neurologists to make their best guess. Or patients can have dementia-like symptoms caused by treatable conditions such as depression, thyroid problems or vitamin deficiencies.
There is no cure for dementia, but early and accurate diagnosis is important. It affects eligibility for research studies and access to support services. Diagnosis determines the likely path of progression and what medications can ease symptoms.
For Lonni, knowledge is power. The teacher in her wants to know why, when and how.
“If you’re a patient, you just keep wondering, ‘What the hell is wrong with me?’ You want it to have a name,” Lonni said. “I want to know why my brain doesn’t work anymore.”
Advertisement
On top of her game
Max Collins was one of 120 students Lonni advised as a professor in health care administration at Minnesota State University. When Collins first met Lonni, he was flunking out. She told him to start working hard or quit and stop wasting his time. “But if you stay,” she said, “I will help you.”
She created a schedule for him, monitored his classwork and eventually helped him get into graduate school.
“She knew what classes I needed to mix together to be able to succeed. She could analyze that and help me balance my life schedule,” Collins said. “She always checked up on me.”
Collins, now 29 and a process improvement specialist at a hospital in Fairbanks, Alaska, credits Lonni with turning his life around.
“She was on top of her game,” he said.

After high school, Lonni Schicker worked as a nurse's aide and a technician in the burn unit at what was then St. John's Mercy Medical Center. She completed the two-year diploma nursing program at Missouri Baptist University in 1983. Here she is shown in her graduation picture. She was 26. Photo courtesy of Lonni Schicker
Former student Samantha McDonald, 29, described Lonni as a professor who could tackle complex topics such as health care finance and use her experience as a nurse and administrator to make it applicable.
“Her teaching was layered under the complexities of health care, which is a tangled web, and she took it step by step to make it make sense,” McDonald said.
After graduating in 2012, McDonald sought out Lonni as a mentor, all while Lonni was developing a master’s of health administration program for the university.
About a year later, McDonald noticed changes. Lonni forgot their meetings for coffee. Her apartment became messy. Her conversations wandered.
Lonni seemed overly sensitive, less professional.
“She was more emotionally charged than usual, almost in a paranoid way,” McDonald said. “She’d always been passionate, but it felt kind of off-the-rocker for her.”
Collins had Lonni as a teacher in graduate school about the same time. She failed to post assignments online. She got the class mixed up with another she was teaching. She didn’t show up.
“We would end up texting her, and she would just cancel,” Collins said. “Or she would come to class, and she would be really disorganized and unplanned.” Lonni blamed stress and other health issues. So did he.
But some students confronted her. They were worried.
Things suddenly became glaring, Lonni said. She got turned around on campus. She lost her spot in a speech about medical ethics that she had given 20 times. She took more time to find the right words.
“I thought I was just overwhelmed with work,” she said.
In late 2013 and early 2014, Lonni was first tested, which involved verbal and written tests. Brain imaging ruled out issues such as strokes or a tumor.

Lonni Schicker's doctorate of education hangs in her bedroom on Wednesday, Feb. 21, 2017. At one time a professor, memory issues forced her to quit and she now works to compile lists of churches. Christian Gooden / St. Louis Post-Dispatch
Test results showed she had difficulty with high levels of functioning such as organization and planning, and an impaired ability to learn new information. Problems were mild, but her records noted: “Change in cognitive ability to the extent evidenced here … will reduce her efficiency and effectiveness in carrying out her responsibilities as she was previously able (as a professor).”
In June 2014, she was diagnosed with mild cognitive impairment. Her neurologist said in his notes that it was unclear whether a “degenerative process” such as Alzheimer’s was responsible. He wanted to see her again in six months.
Lonni says he told her he suspected Alzheimer’s disease. The doctor declined to be interviewed for this story.
His instructions were: Exercise, eat a Mediterranean diet, manage her diabetes, reduce stress, stick with routines, use reminders and “minimize demands on new learning.” He referred her to the Alzheimer’s Association for emotional and educational support.
As part of a research study, Lonni underwent a spinal tap to have her spinal fluid analyzed, which could have helped confirm or rule out Alzheimer’s. The sample got lost in transit, she said.
Unsure of her future and worried, she decided that fall to return home to St. Louis.
McDonald recalls Lonni telling her that people can get through anything if they know how long it will last — such as a challenging semester or a lease on a crummy apartment.
But the mild impairment diagnosis unraveled Lonni’s life of organized plans, timetables and checklists.
“She felt like there was no end in sight … there were so many unknown things about her health and moving and how to pay for stuff and what was happening to her career,” McDonald said. “It’s the only time I’ve seen her in total chaos.”
Advertisement
She used to be a fighter
Once she was approved for Social Security disability, there was a two-year wait for Medicare. In the interim, she was on Medicaid, which meant seeing doctors at clinics where she saw a different doctor every time.
With a high monthly deductible, her overall health worsened. Neurology residents — doctors in training under supervision — staffed the clinic. She said she felt they were blaming her memory problems on depression, diabetes, sleep problems or medications.
“Every time, I saw someone different, they gave me a different conclusion,” Lonni said. “It’s almost as if you leave the physician’s office feeling like you’re making it all up, like they distrust what you say.”
“It's almost as if you leave the physician's office feeling like you're making it all up, like they distrust what you say.”
No one knew what she was like before, how she juggled long work hours, classes and raising a child. No one knew the driven and fiercely independent professor. To her, no one other than Dan understood how her life had completely changed.

Lonni Schicker prepares a big holiday dinner on Sunday, Dec. 17, 2017, as her son Dan sits nearby in their Fenton living room. Cooking the meal is an outlet for Lonni, who encouraged Dan and his friends to gather at their house when Dan was growing up. She can no longer cook when she is alone. Dan has to be at home or on his way before she can start working the stove. Christian Gooden / St. Louis Post-Dispatch
Dan, 31, has to pay her bills and tell her when to take medications. She won’t cook until he’s on his way home from work, scared she’ll forget to turn off burners. She recently stopped driving.
She spends her days inside cleaning, working on crafts and looking up churches for a directory printing company as a part-time job.

Lonni Schicker leaves the Fenton apartment she shares with her son on Friday, Feb. 23, 2018, to drive to the Ballwin office of Guide Book Publishing. She usually works from home but goes to the office occasionally to check in with her boss. Christian Gooden / St. Louis Post-Dispatch
She’s fragile. A person she perceives as rude brings devastation. Everything — from burning a roast to dirty floors — is a crisis. Last fall, she became so anxious she put herself in a hospital psychiatric unit for three days.
“She used to be a fighter. If you disrespected her, she had no problem fighting back. She had no fear,” Dan said. “Now, if she gets a little overwhelmed, she’s in tears.”
“You have dementia. I'm as certain on that as I am of anything. They don't see you like I have. They haven't seen you for the past five years.”
About a year and a half ago, Lonni began volunteering for the Alzheimer’s Association. She speaks at educational events and fundraisers about her experience and makes calls to others in the early stages of dementia.
It makes her feel like a teacher again, like a fighter.
When her Medicare coverage began last spring, it took until November to get in to see neurologist Dr. Mohamed Babiker Tom Bakhit, known as Dr. Tom, at Mercy Hospital. He wanted her to undergo testing once again.
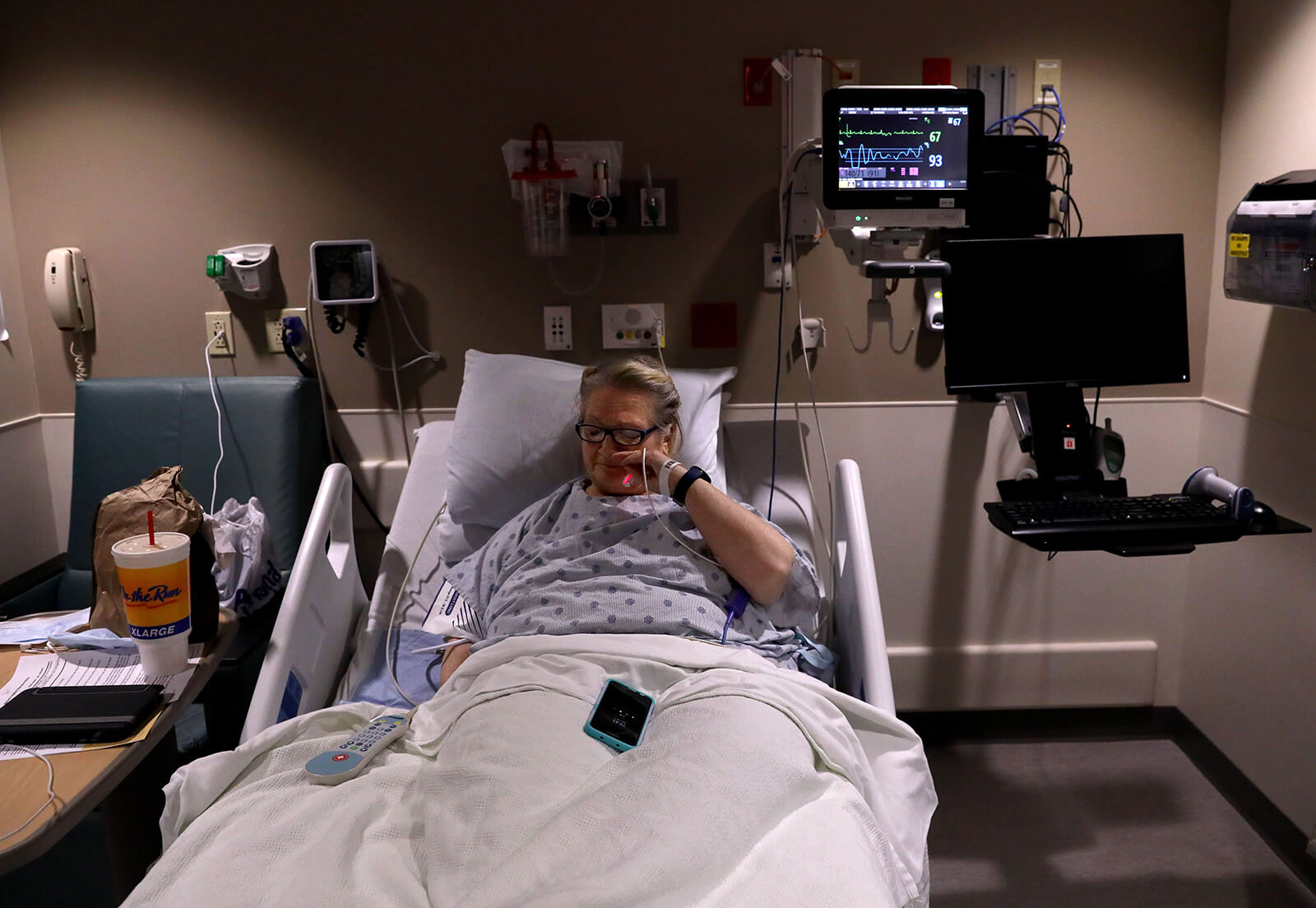
Lonni Schicker settles into her bed at Mercy Hospital in Des Peres after having chest pains on Thursday, Feb. 1, 2018. She was to undergo a round of stress tests the next day. Dan Schicker, her son, came after work. Christian Gooden / St. Louis Post-Dispatch
One early Sunday morning in December, Lonni unraveled. She thought he and others didn’t believe her. She woke up Dan, sobbing. “I’m a fraud,” she said. She should quit volunteering, she told him. She should quit sharing her story. As he always does, Dan calmed her down.
“You have dementia. I’m as certain on that as I am of anything,” he told her. “They don’t see you like I have. They haven’t seen you for the past five years.”
Advertisement
Highest-functioning first
About 16 percent of people in the U.S. age 60 and over — or 11.6 million people — have mild cognitive impairment, according to a new report by the American Academy of Neurology. Studies estimate that an average of 38 percent will develop dementia.
Those under the age of 65 face particular challenges in finding answers to their thinking problems, said Deb Bryer, the early onset support services manager at the association’s Greater Missouri chapter. No one is considering that their unusual symptoms could be dementia.
Changes in personality along with memory problems are early signs, but they are insidious, Bryer said. “What they are experiencing doesn’t send them running to a neurologist.”
Though a diagnosis of mild cognitive impairment can lead to more questions, it is important to recognize.
Often an employer is the first to notice changes, Bryer said. The employee starts getting bad reviews or not completing assignments or directions as quickly. Many quit or get fired.
“People just think they have lost the ability to do their job well,” she said.
People may spend months seeking help for depression until they consider dementia. Divorce and severed relationships are not uncommon, she said. Loved ones don’t understand the odd spending or strange behavior.
Some falsely believe the person is lazy and avoiding responsibilities, trying to annoy them or wanting attention.
“People usually walk through our door pretty demoralized,” Bryer said.
Many do not seek a specialist for testing until dementia becomes obvious: They’ve had several car accidents, wandered off or forgotten names.
Dementia tends to affect the highest-functioning parts of the brain first, so it may be more obvious in a college professor versus someone who’s been chronically unemployed, experts say. Dan thinks his mother could have continued to work, hiding her problems. “But she knew she couldn’t give students the best she had,” he said.
“I can’t imagine how frightening that can be when you are fully aware of your symptoms.”
Tom, her neurologist, said he often saw people in denial, irritated that a family member had brought them in.
“I don’t know why I’m here,” they tell him.
Then there are people such as Lonni, who know their brain is not the same.
“That can be incredibly frustrating,” Tom said. “I can’t imagine how frightening that can be when you are fully aware of your symptoms.”
Tom will review Wright’s findings and make a final diagnosis. Lonni knows things still might not be certain.
“I will learn to live with it, but I want to do whatever I can to get answers,” she said. “This, whatever is wrong, has destroyed my life.”
Fact box
Top misconceptions about Alzheimer's and dementia
Six common misconceptions about dementia and Alzheimer's disease compiled by specialists at Washington University's Memory Diagnostic Center.
Memory problems are a normal part of getting older.
Yes. However, age-related memory loss has little impact on your ability to do what you want to do. Dementia, on the other hand, is the persistent, disabling decline in intellectual abilities.
Dementia is a mild form of Alzheimer's disease.
No. Dementia involves the progressive loss of memory and thinking abilities. Alzheimer's disease is the most common cause of dementia in those over age 65.
All significant memory problems are caused by Alzheimer's disease.
No. Alzheimer's accounts for 60 percent to 80 percent of dementia cases. Other causes include vascular dementia (occurring after a stroke), Lewy body dementia, frontotemporal dementia, traumatic brain injury, Parkinson's disease and Huntington's disease.
There's no reason to get a diagnosis because dementia can't be treated.
No. There are treatable conditions that mimic dementia and Alzheimer’s, such as depression, hypothyroidism, vitamin B12 deficiency, and kidney or liver failure. A diagnosis also can help patients and families manage the disease.
Alzheimer’s diagnosis is only a guess because it can’t be diagnosed until after death.
Largely true. But there are now tests that can be used on living patients, including spinal taps to test for Alzheimer’s disease-related proteins in spinal fluid and PET scans that show deposits of protein in the brain.
Everyone will get Alzheimer’s disease if they live long enough.
No. Alzheimer’s disease is not inevitable, although the chances of getting Alzheimer’s disease increase with age. At least half of 85-year-olds don't have Alzheimer’s.
Questions
We're interested in hearing from readers who are living with dementia, or caring for someone with dementia. As with any conversation, keep comments polite and refrain from personal insults, foul language or off-topic remarks.
Read more about our commenting guidelines.
About this series

Michele Munz has been a reporter for the St. Louis Post-Dispatch for 20 years, the past nine covering health and medicine. As a health reporter, Munz has won awards for her coverage of midwifery care, an experimental treatment for ALS and the opioid epidemic. She was the St. Louis Newspaper Guild’s 2015 Terry Hughes Award winner.

Christian Gooden has been with the Post-Dispatch since 1999. He is a native of University City and graduate of Cardinal Ritter College Preparatory High School. He earned a degree in journalism from Morehouse College in Atlanta, Ga. He has worked at The Atlanta Journal-Constitution and the Milledgeville (Georgia) Union-Recorder.

Cristina M. Fletes is a staff photographer and videographer at the St. Louis Post-Dispatch. She received a bachelor of fine arts degree in studio art from Louisiana State University in Baton Rouge and a master's degree in photojournalism from the University of North Carolina at Chapel Hill.
Andrew Nguyen
Developer
Josh Renaud
Developer
Beth O'Malley
Audience engagement
Elaine Vydra
Audience engagement
Janelle O'Dea
Data reporter
Hillary Levin
Multimedia producer
Gary Hairlson
Multimedia director
Jean Buchanan
Projects editor
Evan Hill
Print designer
Jennie Crabbe
Copy editor
June Heath
Copy editor
Colleen Schrappen
Copy editor